New Resource To Help Patients Understand Inflammatory Breast Cancer (IBC)

The National Comprehensive Cancer Network (NCCN) recently updated its patient guidelines for Inflammatory Breast Cancer. NCCN guidelines provide transparent, evidence-based, expert consensus recommendations for cancer treatment, prevention, and supportive services.
What is Inflammatory Breast Cancer (IBC)?
Inflammatory breast cancer (IBC) is a rare and aggressive form of breast cancer where cancer cells block lymphatic channels in the breast skin. This causes the breast to look red and swollen, and feel warm or hot to the touch, hence the term “inflammatory”. In the US, inflammatory breast cancer accounts for 1-6% of all breast cancer cases in the United States. The disease tends to be diagnosed earlier in life and more often in women with African ancestry.
“A diagnosis of inflammatory breast cancer can be terrifying for the patient as well as their family. Most people don’t know there are different types of breast cancer and need specific information that is designed for patients to help them understand that treatment will be somewhat different and why that’s important,” said Ginny Mason RN, BSN, Executive Director, Inflammatory Breast Cancer Research Foundation and IBC Patient.
Symptoms and Signs of Inflammatory Breast Cancer (IBC)
The symptoms of IBC can be striking but sometimes start out as a subtle difference from the normal appearance of the breast. However, IBC progresses quickly (over the course of days to a few weeks) and very early on can break away from the initial tumor site and invade local lymphatic and blood vessels. Early diagnosis is therefore particularly important with this type of breast cancer.
Symptoms of IBC include:
- A feeling of breast heaviness
- The breast being warmer than usual to the touch
- Persistent itching
- Breast tenderness or pain
- A feeling of milk being let down (not during breast-feeding). Liquid may leak out of the breast and then crust over.
If you experience any of these symptoms, please contact your physician straight away.
The appearance of the breast can be very different from other types of breast cancer:
- IBC causes a swollen breast (can become 2-3 times the normal size). This can be a rapid change.
- Red skin discoloration. Skin redness, or even a bruised (blue/purple) appearance is common with IBC (involving a third or more of the breast).
- Peau d’orange skin appearance (like an orange)
- Ridging
- Inverted or flattening of the nipple
- Skin thickening
- Swollen lymph nodes may also be present under the arm, near the collarbone, or in both places.
A palpable breast lump may or may not be found with IBC. IBC is frequently not felt and frequently missed on mammography, which is why patients should not ignore the other symptoms if a lump is not found. More sensitive imaging methods such as MRI can highlight IBC in women who have “clear” mammograms or who have highly dense breasts that show up as white on a mammogram.
New IBC Guidelines for Patients
The NCCN patient guidelines offer important information so people understand the latest treatments and their options. The new IBC guidelines for patients explain details of the typical course of treatment: systematic therapy (chemo) to shrink the tumor, surgery to remove the affected breast and axillary lymph nodes, and radiation therapy. In many cases, patients may unfortunately have advanced or even metastatic disease by the time of their diagnosis, often because the initial subtle symptoms and signs have been ignored.
“Having easy access to the NCCN patient guidelines empowers people to advocate for themselves when making tough decisions,” added Mason.
With prompt diagnosis and treatment, inflammatory breast cancer is a treatable condition, and the number of long-term survivors is steadily increasing. Learn more about IBC here.
New surgical guideline leads to lower re-operation rates after lumpectomy surgery
Re-operation rates following breast conservation (lumpectomy and radiation) for early invasive breast cancer have been highly variable historically, mainly because of uncertainty and variability in what surgeons deemed safe.
When a tumor is removed, the specimen is painted with a special ink before it is evaluated by a pathologist. This ink allows the pathologist to clearly see the outer edges, or ‘margins’, of the tissue under the microscope.
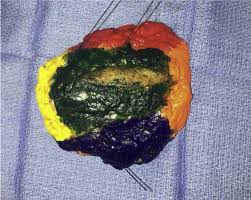
In 2014, the Society of Surgical Oncology and American Society for Radiation Oncology released new guidelines stating that as long as the tumor has no ink on it, the margin is clear. A clear margin means there are no cancer cells at the edge of the surgical specimen and tells the surgeon that all the cancer was removed.
Prior to the new guidelines, some surgeons wanted at least 2mm of normal breast tissue around the cancer. Others accepted less. Even though wider clear margins don’t reduce the risk of cancer recurrence, because of this lack of consensus, 25%-30% of patients having a lumpectomy required more surgery to ensure a larger clear margin.
A recent study in the American Journal of Surgery shows that the new guidelines have led to a decrease in re-operation rates. This offers peace of mind that you likely won’t need another “re-excision” surgery after a lumpectomy if the margins are clear, irrespective of how small the clear margins are, as long as there is “no ink”. Additionally, surgeons now have an evidence-based standard to follow. Very reassuring news indeed!




