Our Cancer Stories
Our Cancer Stories (OCS) is a global cancer resource platform with a database of real patient stories and medically reviewed articles to support patients and caregivers through one of life’s hardest chapters. Our aim is simple: to make the cancer journey feel less lonely and more supported, in ways that recognize each person’s unique needs and lived experience.
Access stories from our database according to your needs, stage, or location, and learn from and be empowered by the experiences of hundreds of patients and survivors— including those navigating breast cancer. We strive to provide up-to-date content informed by the latest research in cancer, global and nationwide guidelines, and clinical practice.
At OCS, we believe that informed patients make better decisions and that no one should have to navigate a cancer diagnosis without the right tools and support. That is why we seek to complement existing resources like the Breast Advocate App, working together towards putting patients at the center of their own care and empowering them to ‘have a voice in their treatment planning‘.
Benefits of a Shared Decision-Making Framework in Breast Cancer Treatment
Being diagnosed with breast cancer can be overwhelming and navigating treatment can be equally or even more challenging. There are many treatment options available, from more conventional treatment methods such as surgery and chemotherapy to novel treatment approaches such as immunotherapy. Patients who have undergone breast cancer surgery may also have to decide if they want to opt for breast reconstruction surgery. Additionally, there may be other considerations depending on each individual patient’s case, such as treatment side effects and implications on quality of life.
Given the sheer volume of information presented to patients, along with the complexity and pressure of decision-making, the experience can be extremely overwhelming. Hence, shared decision-making has become an important aspect of cancer care.
What is shared decision-making (SDM)?
Shared decision-making (SDM) is a collaborative approach to oncology care and healthcare, where both the patient and their healthcare providers assess and review the treatment options together. Through SDM, both patients and their healthcare providers will assess the risks and benefits of the different treatment options as well as patient preferences to help select the best course of action. Unlike traditional approaches to patient care, SDM places a patient’s preference at the forefront and supplements it with the scientific knowledge and expertise of a healthcare professional.
Shared decision-making in breast cancer treatment
In the context of breast cancer care, treatment decisions are incredibly complex. Depending on the type and stage of cancer, breast cancer patients may be presented with a range of surgical treatment options, such as a mastectomy or lumpectomy. Patients may also require adjuvant therapy such as radiation therapy. Additionally, each treatment approach has its own side effects which may impact a patient’s wellbeing.
SDM provides a framework for navigating the complexities of breast cancer treatment decisions, from weighing the pros and cons to aligning choices with the patient’s values and preferences.
Benefits of shared decision-making
Improved patient satisfaction
Studies have shown that SDM improves patient satisfaction, which in turn improves treatment adherence. By allowing patients to choose a treatment approach that best aligns with their personal values and goals, they gain more confidence as they feel more in control of their own decisions. As a result, patients are more likely to adhere to their treatment which in turn, improves treatment outcomes.
Reduced decisional conflict
Decisional conflict refers to the uncertainty about a course of action and is often associated with negative feelings such as anxiety. This could take an emotional toll on some patients, negatively impacting their psychological well-being. In some cases, it may even lead to mental health conditions, such as anxiety disorder and depression. By reducing decisional conflict and the associated psychological impacts, SDM improves a patient’s emotional well-being, as they feel well-supported and informed.
Improved communication
Communication between patients and their healthcare providers plays a crucial role in cancer treatment. It is important to establish a strong foundation of trust and rapport between patients and doctors as it allows doctors to better cater to their patients’ needs.
Studies have shown that a good doctor-patient relationship built upon effective communication supports patient recovery and alleviates their emotional concerns. Conversely, poor communication leads to patient dissatisfaction and an increase in medical disputes. Through SDM, patients and doctors can establish a strong collaborative relationship as they discuss and address the different aspects of treatment.
Shared decision-making tools
Patient decision aids (PDA) are evidence-based clinical tools designed to support SDM. They come in different forms, such as printed materials or interactive online programs. PDAs typically provide evidence-based information on treatment options, the risks and benefits, as well as treatment outcomes. This helps to better prepare patients for their treatment.
Patient decision aids for breast cancer
PDAs for breast cancer can help facilitate decision-making in breast cancer patients. For instance, many breast cancer patients struggle to decide between breast-conserving surgery and mastectomy.
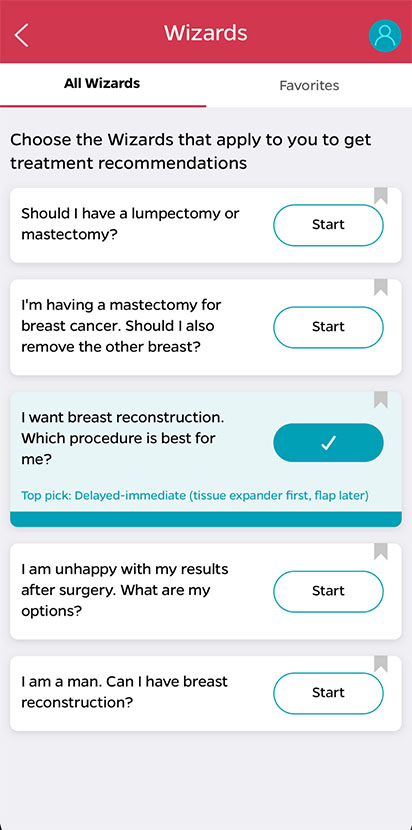
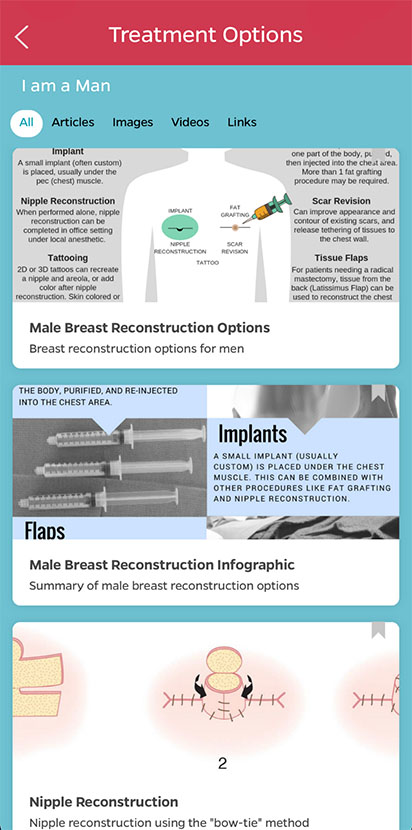
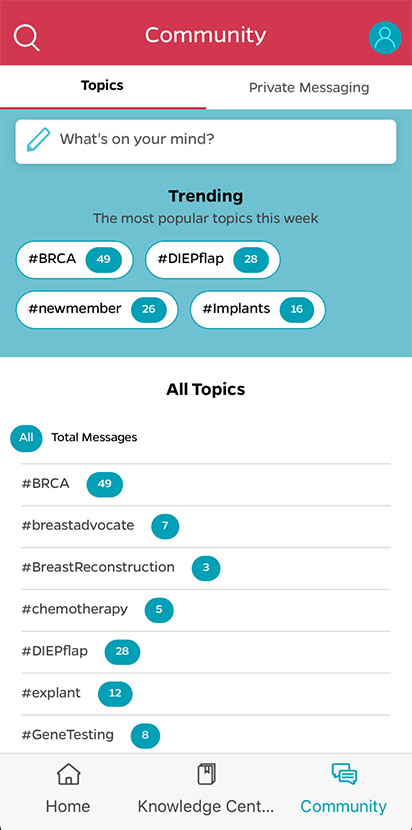
The use of PDAs, such as the Breast Advocate Application, can support and guide patients through such decisions. The Breast Advocate application is the first shared decision-making app for breast cancer surgery and breast reconstruction, which provides evidence-based information and customized recommendations based on patient diagnosis, personal preferences and values. The application can act as a bridge between clinical evidence and a patient’s personal values, helping patients to feel more confident about their treatment decision.
SDM is an approach which allows the patient to be autonomous in their decision while ensuring that their choices are informed by strong clinical foundations. With the ever-evolving nature and complexity of breast cancer treatment, integrating SDM into breast cancer treatment not only improves treatment outcomes but also improves the well-being of breast cancer patients.
This article was created in collaboration with Our Cancer Stories and is intended for educational purposes.
Sources
American Cancer Society. Anxiety
Bruch, J. D., Khazen, M., Mahmic-Kaknjo, M., Légaré, F., & Ellen, M. E. (2024). The effects of shared decision making on health outcomes, health care quality, cost, and consultation time: An umbrella review. Patient Education and Counseling, 129, 108408. https://doi.org/10.1016/j.pec.2024.108408
Chen, X., Liu, C., Yan, P., Wang, H., Xu, J., & Yao, K. (2025). The impact of doctor-patient communication on patient satisfaction in outpatient settings: implications for medical training and practice. BMC Medical Education, 25(1), 830. https://doi.org/10.1186/s12909-025-07433-y
Hoque, F. (2024). Shared Decision-Making in Patient Care: Advantages, barriers and potential solutions. Journal of Brown Hospital Medicine, 3(4), 13–15. https://doi.org/10.56305/001c.122787
Lillie, S. E., Partin, M. R., Rice, K., Fabbrini, A. E., Greer, N. L., Patel, S. S., MacDonald, R., Rutks, I., & Wilt, T. J. (2014). The effects of shared Decision making on cancer Screening – a systematic review. NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK310872/
McAlpine, K., Lewis, K. B., Trevena, L. J., & Stacey, D. (2018). What is the effectiveness of Patient Decision AIDs for Cancer-Related Decisions? A Systematic Review Subanalysis. JCO Clinical Cancer Informatics, 2(2), 1–13. https://doi.org/10.1200/cci.17.00148
Montori, V. M., Ruissen, M. M., Hargraves, I. G., Brito, J. P., & Kunneman, M. (2022). Shared decision-making as a method of care. BMJ Evidence-based Medicine, 28(4), 213–217. https://doi.org/10.1136/bmjebm-2022-112068
Søndergaard, S. R., Bechmann, T., Maae, E., Nielsen, A. W. M., Nielsen, M. H., Møller, M., Timm, S., Lorenzen, E. L., Berry, L. L., Zachariae, R., Offersen, B. V., & Steffensen, K. D. (2024). Shared decision making with breast cancer patients – does it work? Results of the cluster-randomized, multicenter DBCG RT SDM trial. Radiotherapy and Oncology, 193, 110115. https://doi.org/10.1016/j.radonc.2024.110115
Williams, T., Fine, K., Duckworth, E., Adam, T., Bozigar, C., McFarland, A., Nguyen, A., Coles, B. M., & Galiano, R. D. (2025). Patient decision aids in breast surgery and breast reconstruction reduce decisional conflict: a systematic review and meta-analysis. Breast Cancer Research and Treatment, 213(1), 1–14. https://doi.org/10.1007/s10549-025-07752-0
Back to Partners & Resources