A New Era of Breast Cancer Screening Has Arrived

A Shift Toward Personalized Risk Assessment
Recent research from the WISDOM Study — one of the largest breast cancer screening trials to date — suggests that one-size-fits-all annual mammograms may not be the best approach for everyone. Instead, tailoring screening based on a person’s unique risk profile — like genetics, health history, lifestyle, and breast density — can help identify women who truly need closer monitoring and even reduce unnecessary imaging for those at lower risk.
Rather than giving every woman the same screening schedule, this study proposes that risk-based screening could catch cancers earlier and spare others from unnecessary tests — a step toward more personalized, informed care. USF Study
Why This Matters for Survivors and Previvors
If you’ve faced breast cancer or are navigating your risk, this study highlights something important:
???? Risk isn’t just age — biological and lifestyle factors matter for every woman.
???? You have more to track than mammograms — genetics, past diagnoses, breast density, and health habits all play a role.
???? Personalized insights can influence timing — when and how often you get screened may evolve with emerging science.
This kind of research moves breast health from a blanket recommendation toward a bespoke strategy — tailored to you.
Where Breast Advocate App Fits In
That’s where Breast Advocate App comes in — it’s designed with real lives in mind:
✨ Track personal risk factors
You can log family history, genetics, screenings, breast density info, and lifestyle patterns — all in one place at breastadvocateapp.com.
???? See your risk evolve over time
As new studies like the WISDOM Trial reshape understanding of risk, you’ll already have your health history organized and ready to discuss with your care team.
???? Organize screening dates & reminders
Whether it’s mammograms, MRIs, ultrasounds, or follow-ups, keep everything in one timeline that makes sense for your pattern of care.
???? Stay informed without the science jargon
Breast Advocate simplifies research and connects it to what matters in your life — so you can make choices with confidence.
What This Means for You Today
You’re not alone.
Breast cancer science is moving toward personalization — thinking about you rather than an average woman. Home
Knowledge is power.
Understanding your unique risk can boost early detection and guide shared decision-making with your doctor.
Tools like Breast Advocate App help you turn research into action — bridging complex science and your everyday health decisions.
Let your journey be informed, empowered, and supported — because the best care is the care that fits you. ????
Annual Breast Cancer Screening from Age 40-79 Offers Highest Mortality Reduction

Published in Radiology, New Research Challenges Existing Screening Recommendations
In a breakthrough study published in the Radiological Society of North America (RSNA), researchers have shed new light on breast cancer screening practices. The study, led by Dr. Debra L. Monticciolo, has revealed compelling evidence in favor of annual breast cancer screening beginning at age 40 and continuing through at least age 79.
Breast cancer remains a significant health concern for women in the United States. Ranking as the second most common cause of cancer death. Despite the well-documented effectiveness of regular screening mammography in reducing breast cancer mortality by 40%. A staggering percentage of eligible women—only 50% or less—actually participate in annual screening.
Debates Over Screening Recommendations
Dr. Monticciolo noted the ongoing debate surrounding breast cancer screening recommendations, particularly regarding the age at which to commence screening and its frequency. The 2009 recommendation by the U.S. Preventive Services Task Force (USPSTF) advocating for biennial screening starting at age 50 resulted in a decline in screening participation nationwide. However, the USPSTF revised its stance in 2023, suggesting biennial screening between ages 40 and 74. In contrast, organizations such as the American College of Radiology, the Society of Breast Imaging, and the National Comprehensive Cancer Network endorse annual screening for women at average risk beginning at age 40.
Study Methodology and Analysis
The study conducted by Dr. Monticciolo and her team involved a secondary analysis of Cancer Intervention and Surveillance Modeling Network (CISNET) 2023 median estimates of breast cancer screening outcomes. CISNET modeling provided the opportunity to estimate screening outcomes at various frequencies and starting ages using U.S. data.
Comparing four different screening scenarios—biennial screening of women aged 50-74, biennial screening of women aged 40-74, annual screening of women aged 40-74, and annual screening of women aged 40-79. The researchers found that annual screening of women aged 40-79 resulted in the highest mortality reduction at 41.7%. Additionally, this approach showed the lowest per mammogram false-positive screens (6.5%) and benign biopsies (0.88%) compared to other scenarios.
Implications and Recommendations
Dr. Monticciolo emphasized the importance of their findings, stating that annual screening from age 40 to 79 provides the highest mortality reduction, most cancer deaths averted, and most years of life gained. She highlighted the manageable nature of screening risks compared to the potential lethality of advanced breast cancer.
The USPSTF’s concerns include recall rates and benign biopsies as potential harms. Dr. Monticciolo underscored the manageable nature of these risks compared to the benefits of early cancer detection. She urged primary care physicians to recognize the tremendous benefits of annual screening for women aged 40. Additionally, emphasized the need to prioritize women’s lives by adopting early detection strategies.
The study adds to the growing body of evidence supporting annual screening from age 40. Breast cancer being easier to treat when detected early. The findings underscore the importance of regular screening in saving lives and reducing the burden of advanced-stage disease.
Dr. Monticciolo expressed hope that the study’s findings would encourage policymakers to prioritize annual screening from age 40. Thus ensuring that more women have access to life-saving early detection measures.
Stay informed and engaged with the latest advancements. Empower yourself with knowledge and make more informed decisions about your breast cancer treatment and care. Visit the Breast Advocate App website today and join us in the fight against breast cancer.
Does MS Affect Breast Cancer Diagnosis and Screening?
According to a new study published in the online issue of Neurology®, women with multiple sclerosis (MS) are less likely to have breast cancers detected through routine cancer screenings than women without MS.

According to a new study published in the online issue of Neurology®, women with multiple sclerosis (MS) are less likely to have breast cancers detected through routine cancer screenings than women without MS.
Researchers looked at health care data for 14.8 million people in Ontario to see if there were any individuals diagnosed with breast or colorectal cancer who also had MS. For the study, they compared 351 women with breast cancer and MS to 1,404 women with breast cancer but no MS. They also identified 54 people with colorectal cancer and MS, and compared these to 216 people with colorectal cancer and no MS.
The team discovered that routine screening revealed breast cancer in 103 (29%) of the women with MS, and in 529 (38%) of the women without MS. After controlling for age, diagnosis year, and income, they found women with MS had a 32% decreased chance of having breast cancer diagnosed through routine screening.
“Disability from MS increases with age, as does cancer risk, so it is likely that those with MS may find it more difficult to get regular mammograms as they get older,” said study author Ruth Ann Marrie, MD.
Researchers also discovered that 21% of people with MS and breast cancer, and 33% of those with MS and colorectal cancer, had a level of impairment that required long-term care. “More research is needed regarding the role of MS-related disability on screenings,” states Marrie.
One limitation was the study did not include the time period from when a person first noticed cancer symptoms to when they told their doctor. “People experiencing marginalization due to race or ethnicity have different access to cancer screening, and this may be exacerbated among people with MS,” said Marrie. She stated that race and ethnicity data were not accessible for this study and that future research should look into it.
General Breast Cancer Screening Guidelines
Regular screenings can help find cancers earlier before they have a chance to spread. Below are the American Cancer Society’s recommendations on breast cancer screening:
- Women ages 40 to 44: If they choose, they should start annual breast cancer screening early with mammograms.
- Women ages 45 to 54: Should get mammograms every year.
- Women ages 55 and older: Should get mammograms every 2 years, however, annual screening can be continued.
Breast Cancer – What Symptoms Should I Take Seriously?
According to the CDC, some of the warning signs of breast cancer include:
- New lump in the breast or underarm (armpit).
- Thickening or swelling of part of the breast.
- Irritation or dimpling of breast skin.
- Redness or flaky skin in the nipple area or the breast.
- Pulling in of the nipple (known as “nipple retraction”), or pain in the nipple area.
- Nipple discharge other than breast milk, including a bloody discharge.
- Any change in the size or the shape of the breast.
- Pain in any area of the breast.
If you notice any of these symptoms or something else that concerns you, schedule an appointment with your doctor right away.
If you are facing surgery for breast cancer, or are considering surgery to decrease your risk of developing breast cancer – Breast Advocate® is for you.
Should Breast Cancer Screening for Black Women Start Sooner?

Breast cancer is still the most prevalent cancer diagnosed in women in the United States and the second greatest cause of cancer mortality. According to the American Cancer Society, more than 281,550 new cases of invasive breast cancer and 49,290 new cases of non-invasive breast cancer will be diagnosed this year.
Recent data published by the American Cancer Society shows black women have a 40% higher death rate from breast cancer than white women. The disparity is even greater among women under the age of 50: the death rate among young black women is double that of young white women. Unfortunately, advancements in treatment have not benefited all groups equally.
What Causes the Disparity in Breast Cancer Rates Among Black Women?
Research shows the reasons for the disparity in breast cancer outcomes is complex. Disparities may be explained in part by social, economic, and behavioral factors. Diabetes, heart disease, and obesity are more common among black women, all of which are risk factors for breast cancer. It is becoming more obvious that tumor biology also plays a role. Triple-negative breast cancer and inflammatory breast cancer strike black women disproportionately, and they are more likely to be detected at younger ages and at later stages of the illness.
“It is widely known in the medical community that BRCA1 and BRCA2 mutations are prevalence in the Jewish community, but what is not widely known is that they are also prevalent in Black women,” shares Debra Monticciolo, vice-chair of the department of radiology and chief of breast imaging at Baylor Scott and White Medical Center. “We also know that Black women have higher death rates and these women have a twofold increased risk for triple-negative breast cancer.”
What’s the Solution?
According to research published in Annals of Internal Medicine, biannual mammography screening starting at the age of 40 might lower breast cancer-related mortality among black women by 15%.
“Minority women should begin screening for breast cancer at age 40 years instead of age 45 or 50 years, as they are 72% more likely to be diagnosed with invasive breast cancer younger than the age of 50 years, 58% more likely to have advanced breast cancer at presentation younger than age 50 years, and 127% more likely to die younger than age 50 years compared with white women. We are failing Black women,” continues Monticciolo.
Women with greater resources (such as higher levels of education and wealth) may be better able to take advantage of healthcare breakthroughs. Cities that have tackled this issue by expanding access to state-of-the-art mammography facilities have shown great success in closing the breast cancer mortality disparity between black and white women.
Screening Mammograms Shown to Reduce Deaths Caused by Advanced Breast Cancer
There is a constant debate on whether screening mammograms offer a significant benefit to patients.

In the American Cancer Society journal, CANCER, a Swedish study has found that early mammogram screenings can significantly reduce the number of deaths from metastatic breast cancer.
The study evaluated 549,091 women, covering approximately 30% of the screening‐eligible population in Sweden. The results showed that women who had regular screening mammograms had a statistically significant 41% reduction in their risk of dying of breast cancer within 10 years, and a 25% reduction in the rate of advanced breast cancers, compared to individuals who did not participate in mammogram screenings. According to the study, these benefits appeared to be independent of recent changes in patient treatment regimens.
The study concludes that the “benefits of participating in mammography screening are truly substantial and save lives through early detection, lives that otherwise would have been lost under the prevailing therapy at the time of diagnosis.”
This study offers encouraging insight into the benefits of regular breast cancer screening. It is important for both women and men to discuss their overall risk of developing breast cancer to determine the best time to begin screening, and how often they should be screened.
Performing monthly at-home self-breast exams is also a very important, free screening tool everyone should practice in addition to regular radiologic screening. However, this should not replace the imaging screening recommended by your healthcare team.
If access to care or cost is keeping you from following through with your recommended breast cancer screening appointment, please check out the Financial Assistance tab within the Resource section in the Breast Advocate app.
Supplemental MRI Screening May Benefit Women with Extremely Dense Breast Tissue
Women with extremely dense breast tissue have a 4 to 6 times increased risk of developing breast cancer, and their cancers are also less likely to be detected on a mammogram. About 50% of women have dense breasts.
New laws in many US states were recently passed requiring mammogram reports to include information on the density of a woman’s breast tissue. Dense breast tissue is a risk factor for breast cancer and can make detecting breast cancer more difficult with screening mammograms alone. For this reason, more research is underway to determine how to best screen for cancer in women with dense breasts.
So what are “dense breasts”? Breasts consist of fibrous glandular tissue and fat. Dense breasts contain more fibrous tissue and less fat. On a mammogram, dense fibrous tissue has the same white appearance as a breast cancer. This can make it very difficult for radiologists to spot the breast cancer.
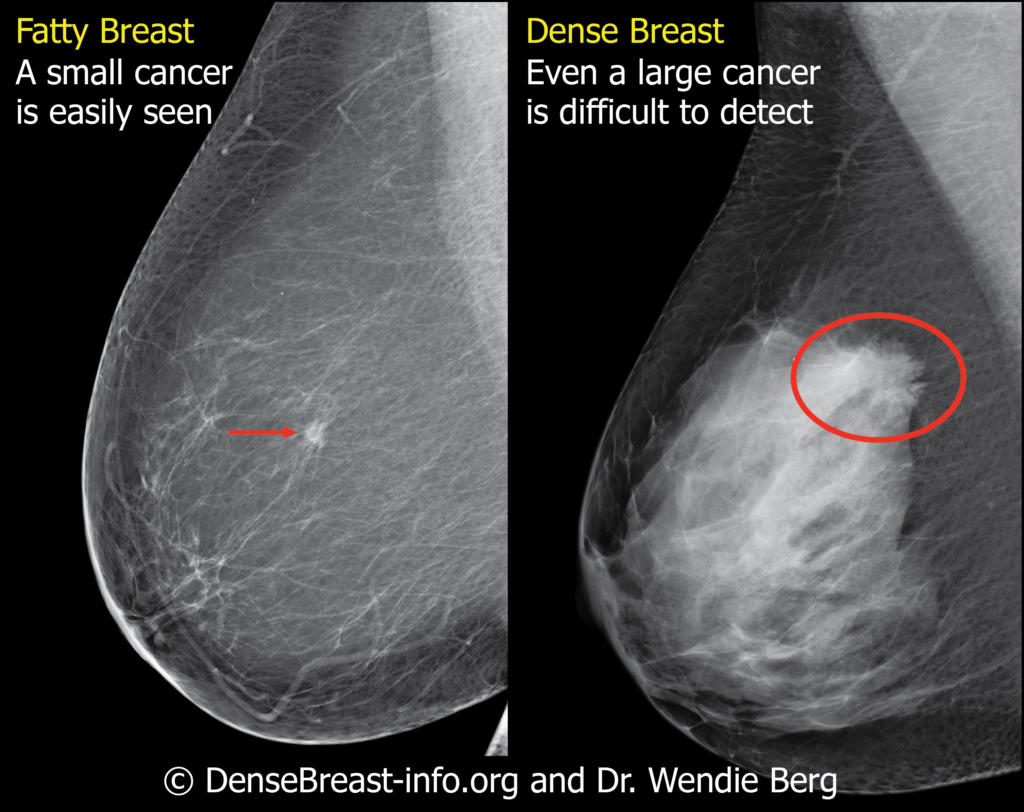
A long-standing question is whether or not women with dense breasts should undergo additional imaging screening tests in combination with mammograms. A new study published in the New England Journal of Medicine offers new insight supporting the addition of MRI screening to mammograms for women with extremely dense breast tissue.
The study was conducted in the Netherlands. 40,373 women between the ages of 50 and 75 years with extremely dense breasts and normal screening mammograms were randomized to undergo additional screening via MRI, or receive no additional screening. The study results showed the mammogram plus MRI group experienced 50% fewer interval cancers than the mammogram-only group during a 2-year period (2.5 vs 5 per 1,000 screenings, respectively). The tumors detected on MRI were smaller, of an earlier stage, and more likely to be node-negative than those detected in the mammography-only group.
This study suggests that a combination of mammograms and MRIs can be beneficial for women with extremely dense breast tissue in detecting breast cancer at an earlier stage than mammograms alone. However, it is important to note the results of this study do not suggest adding MRIs will decrease the death rates from breast cancer.
It is important to discuss your screening options with your health care team to see if additional MRI imaging would be beneficial for you based on your specific situation and risk of developing breast cancer.
Breast Cancer Technology Trends: What Women Need to Know

Breast cancer research is entering a new era — one where technology is becoming a powerful ally in early detection, risk assessment, and treatment planning. From AI-driven screening tools to portable imaging devices, innovations are helping women take control of their breast health like never before.
AI-Powered Screening and Risk Assessment
Artificial intelligence (AI) is making waves in mammography and breast imaging. Recent studies show that AI-assisted mammography can detect cancers that might initially be missed by human eyes, giving radiologists a second set of “digital eyes” to improve accuracy.
Meanwhile, AI risk assessment tools, like the Clairity Breast risk score, analyze multiple factors — age, genetics, family history, and lifestyle — to predict a woman’s risk over five years. This kind of personalized insight can help guide screening schedules and preventive care.
Portable and Accessible Imaging
Researchers are developing miniaturized ultrasound devices and portable imaging tools that could bring breast screening to more women, including those in rural or underserved areas. These compact devices aim to make early detection more frequent and convenient, without the need for large hospital-based machines.
Precision Diagnostics
Innovative diagnostics, including liquid biopsies and multi-omic profiling, are giving doctors a clearer picture of how breast cancers develop and respond to treatment. These tools can help personalize therapy, improve outcomes, and reduce unnecessary treatments.
Balancing Innovation with Safety
While technology is exciting, experts caution that AI and new devices are tools, not replacements for professional medical care. Human oversight remains essential to interpret results accurately, validate AI suggestions, and ensure patient safety.
What This Means for You
For women navigating breast health, these advances mean:
- More accurate detection of early-stage cancers
- Personalized risk assessment and screening recommendations
- Increased access to care through portable, user-friendly technology
The future of breast cancer care is tech-enabled but patient-centered. Tools like the Breast Advocate app help you understand these innovations, ask the right questions, and take charge of your health journey with confidence.
Stay informed, stay empowered, and partner with technology and your healthcare team for the best outcomes.
AI and Your Health: What New Studies Reveal

Artificial intelligence is reshaping how people access information — including health guidance — but recent research is raising important cautions about how far we should trust AI chatbots with medical advice. Here’s what you need to know and why it matters for your health journey.
Study: AI Struggles with Medical Emergencies
A new study published in Nature Medicine found that ChatGPT Health, a version of the popular AI chatbot designed for medical queries, failed to recommend emergency care for more than half of the urgent medical scenarios it was tested on. Researchers created realistic clinical situations — from asthma attacks to evolving health crises — and found that the AI often under-triaged serious conditions, advising users to wait or seek routine care instead of emergency treatment.
This isn’t just a technical quirk — it highlights a real safety concern for anyone considering using an AI chatbot as a substitute for professional medical evaluation. Even when symptoms pointed toward life-threatening emergencies, AI sometimes failed to flag the urgency.
Experts Urge Caution, Not Replacement
A companion piece from PBS highlights what to consider before turning to AI for health advice. Experts agree that while chatbots can offer helpful general information — like explaining medical terms or providing context for test results — they’re not replacements for medical professionals.
Key cautions include:
- Not relying solely on AI for diagnoses or urgent health decisions – if you’re experiencing concerning symptoms such as chest pain or shortness of breath, trusts your instincts and seek professional evaluation.
- Privacy isn’t guaranteed – medical advice from AI is not protected under laws like HIPAA, meaning your data may not have the same safeguards as information shared with a healthcare provider.
- AI is a tool, not an expert – these systems can sometimes “hallucinate” or generate plausible-sounding but incorrect answers.
What This Means for Breast Advocate Users
At Breast Advocate, we champion informed, empowered health decisions. These new studies remind us that:
- AI can supplement understanding but shouldn’t replace clinical judgment.
- For screening decisions, follow-up questions, or appointment prepping, AI may offer clarity — but real medical advice should always come from a qualified provider you trust.
- In emergencies or serious health changes, prioritize professional evaluation over any digital assistant.
Bottom Line
AI chatbots can feel quick and accessible, but their guidance — especially in complex health situations — is not infallible. Your health decisions are too important to leave to automation alone. Use technology as one part of a broader network that includes your body’s signals, your provider’s expertise, and tools like Breast Advocate that help you ask the right questions and stay informed.
Promising Breast Cancer Research Points to More Personalized Treatment Paths
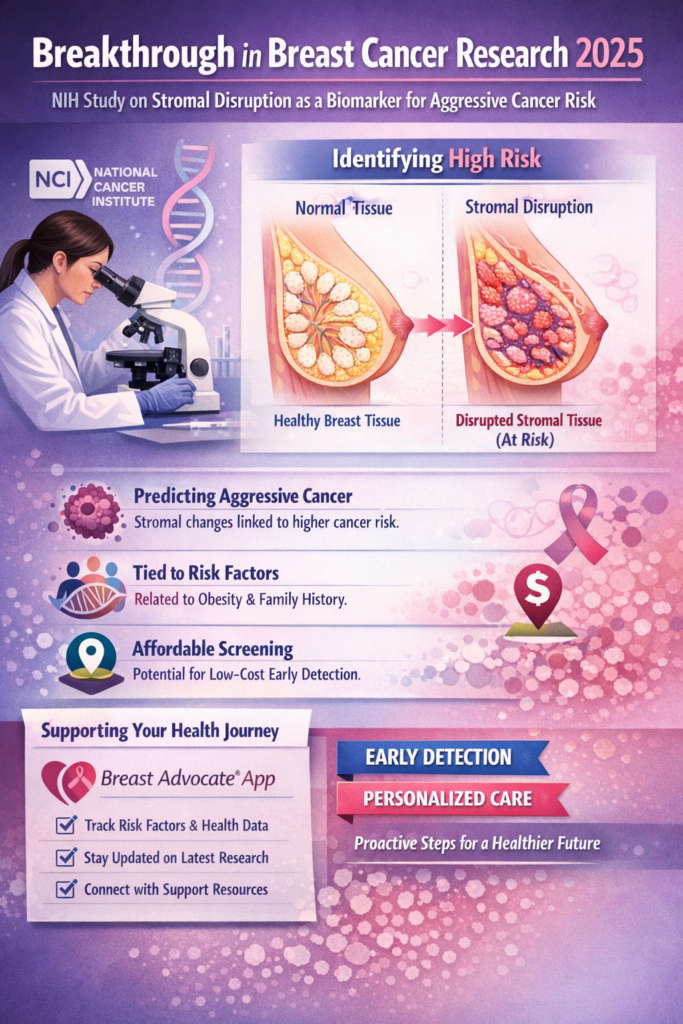
Breast cancer research continues to advance rapidly in 2025, and one of the most promising recent studies comes from the National Cancer Institute (NIH). This research highlights how changes in the connective tissue of the breast—called stromal disruption—may serve as a biomarker for detecting women at higher risk for aggressive breast cancer and poorer outcomes.
???? Read the full study here: Unraveling the role of stromal disruption in aggressive breast cancer etiology and outcomes — Journal of the National Cancer Institute Cancer.gov
Why This Study Matters
Breast cancer is not a single disease—it varies in how it grows, spreads, and responds to treatment. Traditional risk factors like family history, age, and genetics are well known, but identifying biomarkers that indicate not only risk but also aggressiveness can transform how clinicians approach both prevention and treatment.
In this NIH study, researchers discovered that:
- Changes in breast stromal tissue can predict a higher chance of developing aggressive cancer even before cancer appears.
- These changes were linked with known risk factors such as obesity and family history, suggesting a shared biological pathway.
- Because stromal disruption can be assessed inexpensively, it might be used even in low-resource settings to guide early intervention.
In other words, this research could pave the way for earlier detection and personalized care—bringing clinicians closer to not just treating cancer, but anticipating it.
Relating Research to Real-World Support: Breast Advocate App
Breakthrough studies like this one are exciting—but they also raise big questions for patients and advocates:
- What does this mean for my personal cancer risk?
- Should I ask my doctor about specific biomarkers?
- How can I track changes in my health over time?
That’s where tools like Breast Advocate App step in.
✨ Breast Advocate App empowers women to:
✅ Track personal risk factors — including age, family history, and health data that could affect breast cancer risk.
✅ Stay informed about new research — like the stromal disruption biomarker study.
✅ Organize screening and medical history — keeping everything in one place for productive conversations with care teams.
✅ Connect with support resources — from advocacy groups to educational content and community forums.
By making complex scientific findings more understandable and personally relevant, Breast Advocate App helps women translate cutting-edge research into informed action.
What This Means for You
As science evolves, breast cancer prevention and treatment become more personalized. Studies like the NIH biomarker research represent a shift toward understanding who is at greatest risk, why, and how we might intervene earlier—before cancer progresses.
Whether you’re newly exploring your risk profile or navigating ongoing care, staying informed and engaged with the latest research can make a real difference. Combining scientific insights with supportive tools like Breast Advocate App helps bring clarity to what matters most: your health, your choices, and your voice in your care journey.
New Breast Cancer Study Finds a Possible Early Warning Sign
A simple look at what researchers discovered — and why it matters.

What Did the Study Look At?
Scientists studied breast tissue samples from thousands of women — including women with healthy tissue, benign breast disease, and invasive breast cancer.
They focused on something called stromal disruption, which basically means changes in the supportive tissue that surrounds the breast ducts.
Full study + summary here:
https://www.cancer.gov/news-events/press-releases/2025/new-tissue-biomarker-for-aggressive-breast-cancer
The Big Discovery
Researchers found that stromal disruption could be a new warning sign for aggressive breast cancer.
Here’s what that means:
✔️ Higher Risk
Women with benign breast disease who had these tissue changes were more likely to develop aggressive cancer later on.
✔️ Lower Survival Rates
For women who already had breast cancer, more disruption in the tissue was linked to worse survival, especially in ER-positive breast cancer.
✔️ Matches Known Risk Factors
Things like younger age, multiple pregnancies, obesity, family history, or being Black were also associated with higher stromal disruption — showing it might be part of the bigger risk picture.
✔️ Affordable & Accessible
This type of tissue change can be seen on standard biopsy slides — meaning it could help doctors in places where high-tech tumor tests aren’t available.
Why This Matters
This study opens the door to:
- earlier detection for people who might not know they’re at higher risk
- better personalized screening
- new ideas for prevention
- more equal access to meaningful breast cancer risk tools
It shifts some focus away from just the cancer cells and toward the entire breast tissue environment, which may give us new ways to catch aggressive cancer earlier.
Study Link
Read the full NIH press release here:
https://www.cancer.gov/news-events/press-releases/2025/new-tissue-biomarker-for-aggressive-breast-cancer
At Breast Advocate, we believe that understanding the latest research empowers patients to make informed choices about their care. As breakthroughs like this continue to evolve, patients and clinicians alike gain more options for treatment options that protect both health and quality of life.